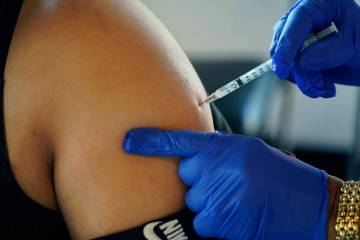
COVID-19 on the run for now, but will it throw another ‘curveball’?
As the delta wave of COVID-19 continues to recede, a note of optimism has crept into the public discussion about the course of the pandemic: Could the worst be behind us?
“I’m hopeful that the worst is behind us, but you never know with variants that are coming forward,” Gov. Steve Sisolak said during a Thursday news conference. “I think that (we’re) making significant progress on the virus and as it relates to delta, which caused our last surge.”
Disease metrics in Nevada, as in much of the country, have been improving since mid-August, after the surge of the delta variant in July.
New cases, hospitalizations and deaths all have declined in Clark County, said Dr. Cassius Lockett with the Southern Nevada Health District. This reflects a pattern seen in other countries of the delta variant burning itself out after two-and-a-half months.
“That’s what we’re banking on,” said Lockett, the district’s director of disease surveillance and control.
Although many health authorities believe the delta wave is nearly done, far less clear is whether a new, fifth wave of COVID-19 could hit as soon as this winter. Some say that depends on factors such as whether more people, including children, get vaccinated and if behaviors such as masking continue.
For many, the most significant factor is whether another dangerous variant emerges.
“It is possible that by late fall or early winter, we could see very substantial downturns in new cases, hospitalizations and deaths, indicating that the virus, contagious as it is, is finding it harder to detect susceptible people,” said Dr. William Schaffner, an infectious disease professor at Vanderbilt University.
“Absent a new rogue variant that can evade the protection of our current vaccines, I think we will be coming to the end, or at least the beginning of the end, of the pandemic phase,” he said, at which point COVID-19 becomes endemic, like the flu.
This disease, however, has been unpredictable.
Delta curveball
Dr. Domenic Martinello, chief medical officer for Southern Hills Hospital, recalls the “collective sigh of relief to be heard across the country” as cases declined in the spring after last winter’s surge.
“Hospital volumes were incredibly low,” he said. “And we thought, ‘This is it. This is great.’ Like, we survived the pandemic, and there might be a couple of scattered cases. And then the delta variant hit.”
“Many of us thought that we were on the homestretch,” Schaffner agreed. “And then delta threw us a curveball.”
He believes the country is better situated now to avoid another surge because of higher numbers of vaccinated people and more people with natural immunity from infection.
“Both are progressively making a larger and larger proportion of our population protected against the virus, or certainly against severe disease,” he said.
But until more of the population is vaccinated, there remains the possibility of another surge, said Karen Duus, a virologist with Touro University Nevada in Henderson.
“People have modeled what’s the best way to ensure that we have the highest variety of variants, and basically, about half the population vaccinated is one of the best ways,” she said.
That is because the evolutionary pressure on variants to escape the immune response makes them become, in effect, smarter.
“If they manage to survive a vaccinated person, and then they get transmitted into an unvaccinated person, then they can just go to town,” she said. “And then they get spread further. And now you have something that takes over, if it’s able to replicate a lot, very well and efficiently, and get transmitted.”
Delta mutants
The director of the Nevada State Public Health Laboratory said the strains that have evolved from the delta variant are increasing in prevalence and that one has shown signs of having a greater ability to elude the immune system.
The lab has identified a case of COVID-19 reinfection in a man in Mineral County just 22 days after his first infection.
The first infection was of the delta variant and the second of a mutant, or sublineage, of the delta variant known as AY.26, the lab’s director, Mark Pandori, told the Review-Journal.
More cases of similar reinfections would need to be identified before the implications of this finding become clear.
But he predicts that sublineages of the delta variant will play a role in the course of the virus.
“And to me, this is going to be how the virus stays in the population until winter, when it’s probably gonna have a lot more of an opportunity to spread,” Pandori said.
There’s no way of knowing when and if a descendent of delta, or any another variant, will emerge to cause a new surge, said Schaffner, the Vanderbilt professor.
“Whether or not a rogue variant shows up is going to be extremely determinative,” Schaffner said. “You can’t predict when, if ever, you’re going to be dealt that card.”
It’s like, he said, predicting where lightning will strike. “It is genuinely a genetic random event.”
Should such a variant emerge, it would be necessary to rapidly create a specific vaccine against that variant, a process made easier by the technology behind the Pfizer and Moderna vaccines.
“Take a deep breath and start over,” he said, envisioning that scenario. “Vaccinate and or boost, if you want to call if that, everyone once again.”
Contact Mary Hynes at mhynes@reviewjournal.com or 702-383-0336. Follow @MaryHynes1 on Twitter.